|
1/20/2024 0 Comments Jock itch female pictures 
Due to its potential for hepatotoxicity, oral ketoconazole is no longer recommended for dermatophytoses. Griseofulvin has similar pharmacokinetic limitations as fluconazole, and it is more appropriately utilized in the management of tinea capitis than tinea cruris. Fluconazole has demonstrated efficacy in treating tinea cruris however, it is not preferred due to its poor keratin adherence and prolonged treatment duration. Oral terbinafine and itraconazole have favorable characteristics for dermatophyte management and are the most often prescribed. Stratum corneum penetration and concentration maintenance, keratin adherence, patient tolerance, and a minimal drug interaction profile are hallmarks of the ideal systemic medication for dermatophytoses. Extensive or diffuse rashes and patients with immunocompromise may also require systemic treatments. Oral preparations exist to manage tinea cruris and are indicated for chronic, recurrent, and recalcitrant disease. Recent studies have demonstrated a number of benefits to ciclopirox therapy however, it remains an underutilized antifungal medication. Ciclopirox olamine is an older topical preparation with a unique mechanism of action compared to the commonly used allylamines and azoles. One newer topical azole, luliconazole, requires only once daily application for one week and may improve patient compliance through a more convenient dosing schedule. Azoles are not as costly as allylamines but often require a longer treatment duration. Allylamines have a potentially shorter treatment timeline, have demonstrated lower relapse rates, and their metabolism is independent of the cytochrome p450 system. ĭeciding which agent to use should be based on patient compliance, cost, and medication accessibility, as there is insufficient data to directly compare the effectiveness of individual drugs and classes. They are generally prescribed once or twice daily for two to four weeks. Allylamines (terbinafine, butenafine, naftifine) and azoles (clotrimazole, miconazole, sulconazole, oxiconazole, econazole, ketoconazole) are the mainstays of topical treatment regimens. 
Topical therapies are effective and usually preferred. Management strategies are similar worldwide however, some countries have specific guidelines based on their region's fungal profile. 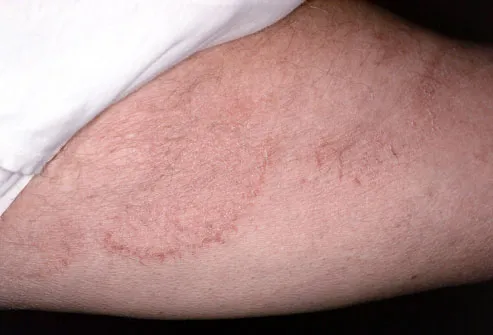
Īntifungals utilized in treating dermatophytoses, including tinea cruris, target the synthesis of ergosterol, a vital component of fungal plasma membranes. Diabetes mellitus, family members with tinea, and personal history of cooking food were found to be positively associated with chronic and relapsing disease. In India, an area affected disproportionately often with dermatophytes, a study was conducted in response to the increasing frequency of and decreased treatment efficacy for local tinea infections. Of all these factors, perspiration appears to be the most influential variable in the development of infection. Genetics can also make a patient more susceptible to dermatophytes. Īthletes, especially those involved in contact sports, may be more likely to contract tinea infections. Several risk factors have been identified that predispose an individual to tinea cruris, including excessive perspiration, occlusive clothing, improper hygiene, diabetes mellitus, immunocompromise, and lower socioeconomic status. Trichophyton rubrum has been isolated most commonly and remains the most frequent cause of tinea cruris worldwide however, most studies do recognize the increasing prevalence of Trichophyton mentagrophytes and other organisms in certain regions. It may mean that the person has a body-wide infection, impaired drainage, or an immune system disorder.Tinea cruris is caused by dermatophytes belonging to three genera, Trichophyton, Epidermophyton, and Microsporum. When more than one area of lymph nodes swell, this is called generalized lymphadenopathy. Swollen lymph nodes in the groin are usually a sign that there is an infection or inflammation in the genitals or lower body, such as the legs or possibly the feet. Doctors refer to this as localized lymphadenopathy.įor instance, swollen lymph nodes in the neck could be a symptom of a cold or the flu. They may be tender or painful.Ī swollen lymph node in one area can signal that there is inflammation or an infection in that specific area of the body. When an infection, inflammation, injury, or other illness affects the body, lymph nodes may swell as they gather the harmful cells and filter them.Ī person may be able to feel swollen lymph nodes by gently pressing on the area. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
